Hydrocele Testis: Modern aspect, Causes, Symptoms, Treatment
Article by Dr Raghuram Y.S. MD (Ay) and Dr Manasa, BAMS
Hydrocele is a term given to explain a ‘pathological accumulation of serous fluid’ in a body cavity. It can happen in any body cavity. But when this happens around the testis, it is called ‘Hydrocele Testis’.
In this article I have used the term hydrocele to explain ‘hydrocele testis’ omitting the other cavities of the body. To avoid repetition I skipped using the term ‘testis’ alongside hydrocele and have just used the term ‘hydrocele’ to explain the condition. Even in general terms, hydrocele is a word used to denote ‘hydrocele testis’ unless specified otherwise.
Table of Contents
Introduction
Hydrocele Testis – It is a condition in which there is accumulation of fluids around a testicle (cavities around the testicle). It is often caused by the fluid secteted by tunica vaginalis, one of the covering layers of the testis. (Tunica Vaginalis is a remnant piece of peritoneum wrapped around the testicle).
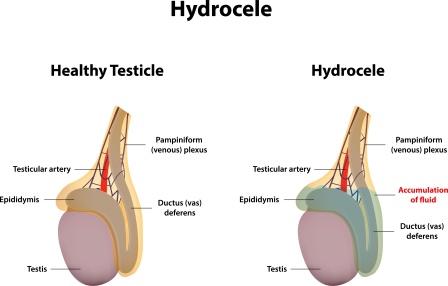
Hydroceles occuring in kids below the age of 1 year usually resolve spontaneously if there is no hernia associated with hydrocele.
Primary Hydroceles – They develop in adulthood. They occur particularly in elderly people and more over in hot countries. It happens by slow accumulation of serous fluid, presumably caused by impaired reabsorption of fluids.
A hydrocele can also be caused by repeated chronic infection of Wuchereria bancrofti or Brugia malayi, two musquito-borne parasites of Africa and Southeast Asia respectively. The infection causes plugging of inguinal lymphatic system which in turn leads to collection of fluid around the testis leading to hydrocele.
Hydrocele can also be a part of more diffuse sequelae referred to as elephantiasis.
Causes
There are 4 ways in which a hydrocele can be produced. They are as below enlisted –
- Due to excessive production of fluid within the sac, example secondary hydrocele
- Due to defective absorption of fluids
- Due to interference with lymphatic drainage of scrotal structures, example as in elephantiasis
- Due to connection with a hernia of the peritoneal cavity (congenital variety), which presents as hydrocele of the cord
Primary Hydroceles
The swelling in primary hydrocele is soft, non-tender.
It is large in size.
Testis cannot be felt (usually)
Presence of the fluid around the testis is demonstrated by trans-illumination test.
Hydroceles are initially painless and as a result are ignored. As a result they can reach a huge size, containing large amount of fluid. The size and weight of the hydroceles cause inconvenience. Otherwise they are asymptomatic.
When diagnosed early, they are small. The testis can be palpated within a lax hydrocele. When left unattended, they can become large.
Secondary Hydroceles
Secondary hydroceles can occur due to testicular diseases. They can be the result of cancer, trauma (such as hernia), or orchitis (inflammation of testis). They can also occur in infants undergoing peritoneal dialysis. This condition is often associated with acute or chronic epididymo-orchitis. It is also seen alongside torsion of the testis and with some tumors of testis.
This type of hydrocele is usually lax and moderate in size. The underlying testis is usually palpable. The condition subsides once the primary lesion (which causes it) resolves.
Below said are the common causes (and associated conditions) –
- Acute / chronic epididymo-orchitis
- Torsion of testis
- Testicular tumor
- Haematocele
- Filarial hydrocele
- Post herniorrhaphy
- Hydrocele of a hernia sac
Infantile Hydroceles
In infants and children, a hydrocele is usually an expression of a patent processus vaginalis (PPV). The processus vaginalis doesn’t connect to the peritoneal cavity.
Congenital Hydroceles
The processus vaginalis is patent and connects with the general peritoneal cavity. The communication is usually too small to allow herniation of intra-abdominal contents. When manual pressure is put on the hydrocele, it usually doesn’t get empty. The hydrocele fluid may drain into the peritoneal cavity when the child is lying down. If the swellings are bilateral, ascites or even ascetic tuberculous peritonitis should be considered.
Encysted hydrocele of the cord
There is a smooth oval swelling near the spermatic cord. The swelling moves downwards and becomes less mobile on gently pulling the testis downwards. Rarely, a hydrocele develops in a remnant of the processus vaginalis somewhere along the course of the spermatic cord. This is called as an encysted hydrocele of the cord. This hydrocele also trans-illuminates like other hydroceles. Ultrasound imaging helps in differentiating hydrocele from a scrotal hernia or tumor.
Clinical diagnosis
A primary hydrocele is described as having the below mentioned characteristics –
- It gives a positive trans-illumination test
- Fluctuation is positive
- Impulse on coughing is negative, unlike hernia (positive in infantile hydrocele)
- Reducibility is absent
- Testis cannot be palpated separately
Treatment
The hydroceles appearing in the first year of life resolve spontaneously without any treatment. Therefore they seldom need treatment.
Those hydroceles which persist after the first year of age or occur later in life need treatment through open operation for removing surgically.
Open operation under anesthesia (spinal of general) is the operation of choice in adults.
In suspected testicular tumor, a hydrocele must not be aspirated. If it is aspirated, the malignant cells can be disseminated via the scrotal skin to its lymphatic field. This is excluded through ultrasonography.
Aspiration – of fluid should be done using a needle and syringe if tumor is not present.
Post-operative care – Scrotum should be supported. Ice bags should be placed to support to scrotum and also to soothe the pain. Surgical dressings should be changed regularly. The drainage of fluid should be regularly observed and noted. A keen observation to see any manifestation of complications will help in recovery and also to prevent re-operation. When one or more complications are present, open operation with or without orchidectomy is preferred.
Jaboulay’s procedure
When aspiration is done for primary hydrocele, the fluid tends to re-accumulate over a period of time. For this, periodic aspiration or operation is needed. Operation is usually preferred for younger patients. In elderly patients or those unfit for operations, repeated aspirations should be done whenever the hydrocele becomes uncomfortably large.
Sclerotherapy is an alternative. After aspiration, 6% aqueous phenol together with 1% lidocaine can be injected. This acts as an analgesic and also prevents re-accumulation.
Aspiration and injection with sclerosing agents, sometimes with Tetracyclines may be necessary.
Complications
- Rupture – usually occurs due to trauma, may also be spontaneous
- Herniation – of hydrocele sac occurs in chronic cases
- Haematocele – Hydrocele may transform into haematocele if there is spontaneous bleeding into the sac or due to trauma. If the haematocele is not drained, a clotted haematocele usually results.
- Calcification of sac – The hydrocele sac may calcify. Clotted hydrocele may result from a slow spontaneous ooze of blood into the tunica vaginalis.
- Infection – Severe infection can be introduced by aspiration occasionally. Aspiration can be used as a temporary measure in cases where surgery is contra-indicated or must be postponed.
- Postherniorrhaphy hydrocele – rare complication of inguinal hernia repair, possibly due to interruption to the lymphatics draining scrotal contents
- Pyocele – infection of sac can cause pyocele
- Atrophy – of testis occurs in long standing cases
Differential diagnosis
Inguinal hernia (groin hernia) – It is a protrusion of abdominal cavity contents through inguinal canal. It occurs when tissue, such as part of the intestine protrudes through a weak spot in the abdominal muscles. It presents as a bulge in the groin or scrotum. It feels like a round lump. It may form over a period of weeks or months or all of a sudden after you have been lifting weights, coughing, bending, straining or laughing. Many people don’t seek treatment because it may not cause any symptoms. The symptoms if any occur as pain in the bulge, especially when you cough, bend over or lift a heavy object.
It is very difficult to differentiate hydrocele from an incarcerated inguinal hernia. A groin ultrasound will help. It shows an abnormal ballooning of the antero-posterior diameter of the inguinal canal suggesting hernia. Occasionally, a segment of omentum (fat) or a segment of the bowel is seen.
Testicular Cancer – Presents as solid, firm masses around the testis which do not trans-illuminate (unlike hydrocele). However tumors may have reactive hydroceles surrounding them which trans-illuminate. Scrotal ultrasound will help in clinching diagnosis. Testicular tumor markers, such as alpha-fetoprotein or beta-hCG, may also indicate tumor activity.
Epididymitis – is an inflammation of the epididymis, a tube near (behind) the testis which stores and carries sperms. It presents with pain and swelling in the testicles, along with pain, tenderness and or discomfort in the scrotum, epididymis or the testicles. Local inflammatory changes can also be seen. The diagnosis can be confirmed using Color Doppler Ultrasonography.
Epididymo-orchitis – It is a condition in which there is inflammation of epididymis and testis. It presents with scrotal swelling and swelling. Clinically the patient has pain and tenderness in the scrotum and local inflammatory changes can be seen. The diagnosis can be confirmed using Color Doppler Ultrasonography.
Epididymal cyst – also called as spermatocele is a painless, fluid filled cyst in the long, tightly coiled tube that lies above and behind each testicle (epididymis). The fluid in the cyst may contain sperm that are no longer alive. It feels like a smooth, firm lump in the scrotum on top of the testicle. This mass can be trans-illuminated. The position of the cyst helps in the diagnosis. The cyst can be palpated separately from the testis, lying posterior and superior to it. Scrotal ultrasound will further help in making a clear-cut diagnosis.
Scrotal edema – is thickening and swelling of the scrotal wall. Scrotal exam and scrotal ultrasound will help in diagnosis of this condition.
Testicular Torsion – occurs when the spermatic cord twists (when testicle rotates, twisting the spermatic cord that brings blood to the scrotum), cutting off the testicle’s blood supply, a condition called as ischaemia. The signs of torsion are extreme tenderness, rapid onset of pain in testicles, elevation of the testis, loss of landmarks, absence of a cremasteric reflex. The diagnosis can be confirmed using Color Doppler Ultrasonography.
Varicocele – It is an abnormal enlargement of the pampiniform venous plexus in the scrotum (this plexus drains the testicles). It may develop as a result of poorly functioning valves that are normally found in veins. In other cases, it may occur from compression of a vein by a nearby structure. This can lead to decreased sperm production and quality leading to infertility. Palpation of enlarged veins during Valsalva maneuver is diagnostic on physical exam. Physical exam is diagnostic, but color Doppler ultrasonography can be used for confirmation.
Related Studies and Researches
Study in Michigan University (2010) – Processed foods that have had the dietary fiber taken out of them will cause difficult and infrequent bowel movements. The consequent constipation puts more pressure on veins, especially when you use the restroom. This worsens the varicocele. When you eliminate these foods from your diet, it would be possible either to prevent or ease the symptoms of varicocele. Low fiber, high processed diet, including white flour goods and sugar contributes to slow bowel movements that forces drying of stools, which in turn cause severe pressure on veins and lead to varicocele.
British Journal of Surgery study (2000) – Flavonoids in the food act to increase venous tone, strengthening the walls of the veins and thereby making them less susceptible to varicocity. Therefore flavonoids should be included in a whole food diet to relieve varicocele. Incorporating flavonoid rich foods like fresh vegetables and fruits is a great way of preventing or relieving the symptoms of varicocele as they immensely contribute to blood vessel health. Moreover, maintaining a ‘whole foods’ diet will improve your overall health and thereby help you relieve your varicocele. So, choose whole grains, fish and poultry, flax seeds, fish oil and other organically grown foods over processed foods. (related)
New York University Study (2007) – Butcher’s broom or Ruscus aculeatus help reduces swelling of veins that cause varicocele. This herb thus can be used to treat Varicosities of the leg (similar condition) also. Other herbal remedies which help to strengthen and tone veins are horse chestnut and bilberry. Thus natural herbal remedies can be used to help treat your varicocele.
Fiber rich diet – Constipation worsens Hydroceles. It causes unnecessary and excessive intra-abdominal pressure that can worsen hydrocele. It also increases the pain. In presence of constipation, one can think of taking steps to relieve the excessive strain needed for bowel movements by following a high-fiber diet. Incorporating fresh fruits, raw vegetables, and whole grains to ensure easy bowel movements and less strain on the hydrocele will help.
Study from University of Missouri (2010) – Horse chestnut is an important natural remedy in healing varicose veins and varicocele. Its extract is found to be effective in healing varicocele and also in improving sperm quality owing to the presence of its active ingredient aescin (escin). Study from University of Missouri (2010) has discovered that men treated with horse chestnut extract saw a marked improvement in their sperm quality after treatment. The study entitled ‘Escin improves sperm quality in male patients with varicocele-associated infertility’ examined 219 men with infertility related to varicoceles.
Click to Consult Dr Raghuram Y.S. MD (Ayu)









